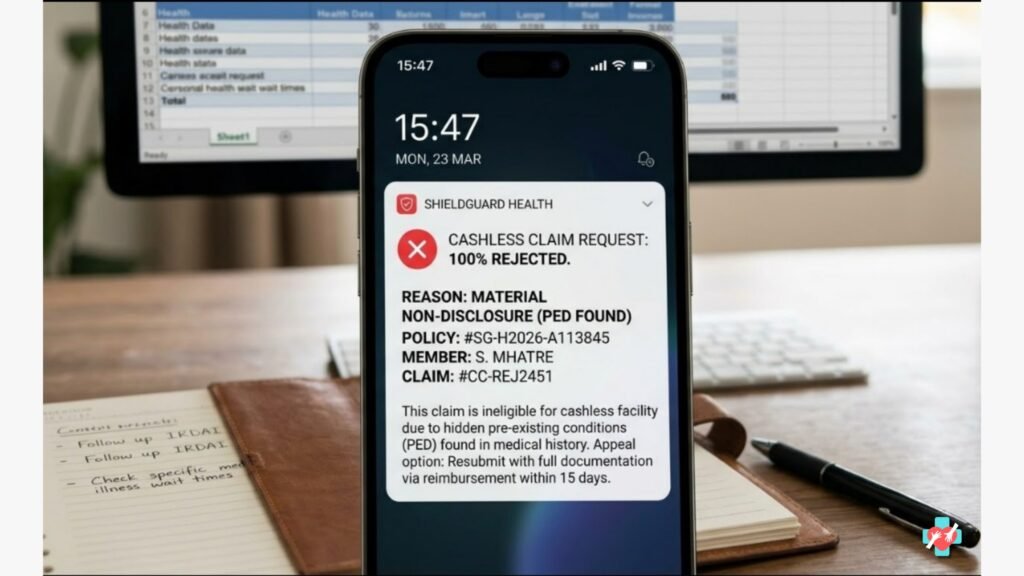
In the insurance industry, an Early Claim is generally defined as any claim filed within the first 1 to 2 years of a policy’s inception.
Because the policy is new, insurance companies view these claims with a high degree of scrutiny. They often suspect that the policy was purchased specifically because the person already knew they were ill—a concept known as “Anti-Selection.”
Here is why early claims face a higher risk of rejection:
- Investigation for non-disclosure
When a claim is filed early, the insurer’s first step is to check if the illness existed before you bought the policy.
- The Logic:If you have a major surgery just 6 months after buying a policy, the insurer may investigate your medical history (via your Aadhaar-linked records or hospital data) to see if you had symptoms or consultations for that issue earlier.
- The Result:If they find any evidence of a pre-existing disease (PED) that wasn’t mentioned in your proposal form, the claim will be rejected for “Material Non-Disclosure.”
- Initial 30-Day Waiting Period
Almost all health insurance policies in India have a mandatory 30-day waiting period starting from the day the policy is issued.
- The Rule:Any claim for an illness (fever, infection, surgery) within these first 30 days is automatically rejected.
- The Exception:Only claims arising from accidents (like a road mishap) are covered from Day 1.
- “Specific Illness” Waiting Periods (1–2 Years)
Many common ailments have a “slow-growing” nature, and insurers impose a fixed 2-year waiting period for them, regardless of whether you had them before.
- Common Rejections:Claims for Cataracts, Kidney stones, Hernia, Piles, or Joint replacements filed in the first or second year are almost always rejected because they fall under the Specific Illness Waiting Period.
- Moratorium Period Rules (New IRDAI Updates)
In India, the Moratorium Period is a protection for the policyholder, but it only kicks in after a certain time.
- Before 5 Years:In the early years (Year 1 to Year 5), the insurer has the full right to investigate and reject claims based on non-disclosure.
- After 5 Years:Once you complete 5 continuous years (reduced from 8 years as per 2024-2026 rules), the insurer cannot reject a claim for non-disclosure unless they prove a massive, intentional fraud.
- Suspicion of “Planned” Hospitalization
If a policyholder is hospitalized for a “vague” reason (like body pain or weakness) shortly after buying a policy, the insurer may reject it as “Unjustified Hospitalization.” They may argue that the treatment could have been done as an outpatient (OPD) and that the patient only got admitted to “use” the new insurance.
How to protect your Early Claim?
- Wait for the 30 days:Avoid claiming for minor illnesses in the first month unless it’s an emergency.
- Be Honest:Disclose every minor health issue (even a cough or BP) during the application so they can’t use “non-disclosure” as a reason later.
- Check Exclusions:Read the “Specific Waiting Period” list in your policy document so you aren’t surprised by a rejection for a surgery like a Hernia in Year 1.
- Reach out to us thru
- Website:-https://herculesadvisors.in/
- Twitter:-https://x.com/NIKHILLJHA
- https://x.com/AdityaD_Shah
- Instagram:-https://www.instagram.com/herculesadvisors/
- Youtube:-https://www.youtube.com/@HerculesInsurance
- Email us on:-nikhiljha159@gmail.com
